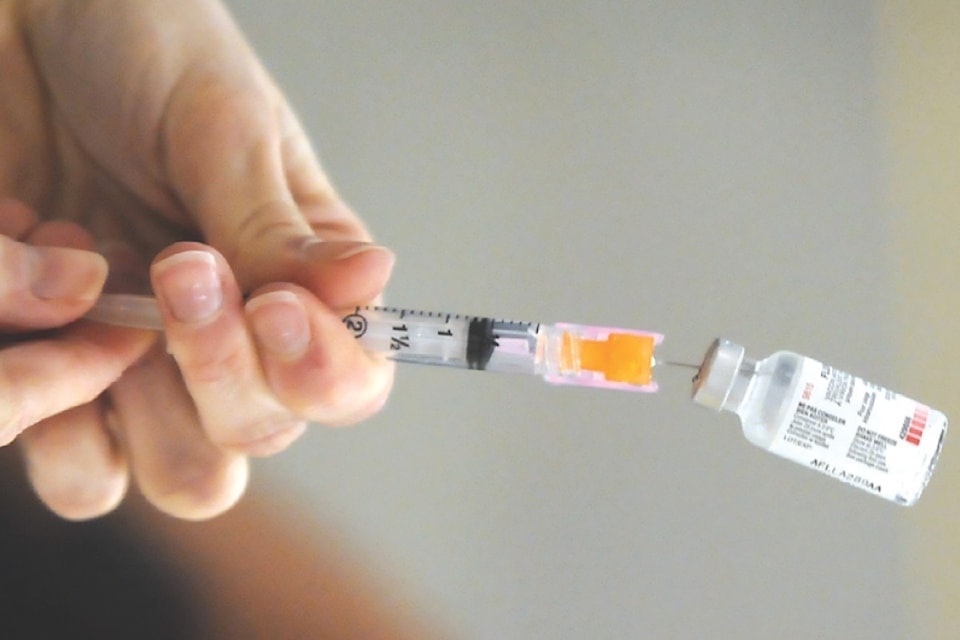
TORONTO – This season’s influenza vaccine is estimated to have been more than 40 per cent effective in preventing illness with the dominant H3N2 viral strain in Canadians who got their shots, a national network of infectious diseases experts says.
The Canadian Sentinel Practitioner Surveillance Network determines vaccine effectiveness by analyzing how many inoculated people tested positive for the flu virus compared to those who were unvaccinated.
“A vaccine effectiveness of 40 per cent against the H3N2 virus is decent,” lead researcher Dr. Danuta Skowronski of the B.C. Centre for Disease Control said Thursday from Vancouver.
“It’s lower than we would like to see, particularly because H3N2 epidemics tend to be associated with more hospitalizations and deaths. But reducing the risk by 40 per cent is really important, not only at the individual level, but also at the population level when we tally the serious outcomes at the end of the season.”
Young children, the elderly and people with underlying health conditions like heart disease are vulnerable to complications from flu; H3N2 flu is particularly hard on the elderly.
An effectiveness level of about 40 per cent means the risk of getting sick enough to require medical attention is almost cut in half, and Skowronski said that’s important for those at risk of complications.
This season’s vaccine, which contained components aimed at preventing illness from two A strains – H3N2 and H1N1 – and a B strain, has been much better at protecting people than the 2014-15 shot, which was mismatched to the H3N2 genetic variant that ended up circulating that season.
The decision on which influenza strains – and which particular genetic variations of those strains – to target in an upcoming flu season is decided by the World Health Organization (WHO) each February, giving pharmaceutical companies time to produce the vaccine.
But in the intervening months, the viruses can genetically mutate, sometimes leading to such a mismatch as occurred in 2014-15.
Skowronski said vaccine effectiveness levels from Canada and other countries, as well as what genetic mutations might have occurred as the flu bug was passed from person to person over the season, help the WHO decide what strains next season’s vaccine should contain.
“There’s a lot of complexity to the influenza virus. We like to think of it as just a uniform beast, but it’s not. It’s constantly changing shape, it’s constantly evolving.”
And from what the surveillance network is seeing, next season’s vaccine could very well be altered.
“There are quite a few emerging variants of H3N2 virus, by province,” she said, noting that genetic decoding of virus samples in Alberta showed a lot of consistency, but B.C.’s cases presented a “rainbow” on a coloured bar graph. “Ontario and Quebec are also showing a smorgasbord of viruses, compared to what Alberta was showing.
“This virus is dynamically evolving, real time, during the epidemic. So there’s variation … that’s showing up in this virus as it’s trying to evade the immunity in the population.”
That variation was reflected in vaccine effectiveness in different regions of the country. In Alberta, where influenza activity started earliest and where there was a single dominant H3N2 variant, the shot’s effectiveness was estimate at about 60 per cent. In B.C., Ontario and Quebec, where flu activity was delayed and a greater mix of H3N2 genetic variants was detected, the estimate was about 30 per cent.
As of Jan. 28, 12,694 laboratory-confirmed influenza cases had been reported to the Public Health Agency of Canada, according to the most recent figures from its FluWatch report. However, that number represents the “tip of the iceberg” as most people who get a flu-like illness don’t seek medical attention, experts say.
There had also been 2,964 hospitalizations and more than 105 deaths, most of them among adults aged 65 or older.
Skowronski said H3N2 has been responsible for 95 per cent of flu cases this season, but the number of new infections with that viral strain has now begun to wane.
“It does look like generally we’ve turned the corner on this H3N2 wave, we’re likely on the down slope of the epidemic curve – just,” she said.
“And now … we’re starting to pick up some influenza B activity – not much, but it’s starting – and we do often see a tail-end wave of influenza B, so now we’re waiting to ride that wave out to the end of the season.”
The research was published online Thursday in the journal Eurosurveillance (http://eurosurveillance.org/).
– Sheryl Ubelacker, The Canadian Press