It’s been a long and bumpy road, but Maureen Kennah-Hafstein’s 13-year journey may finally be reaching smoother ground.
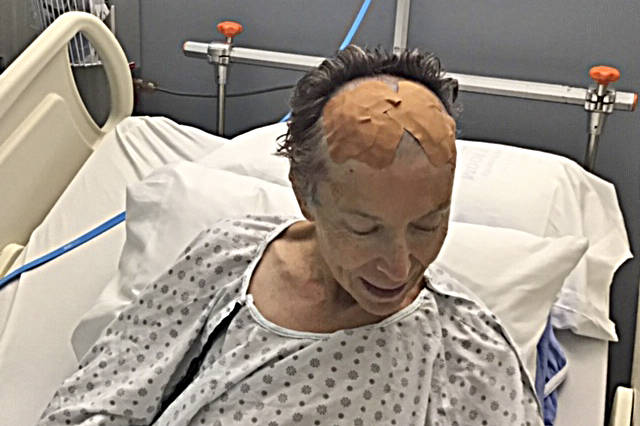
On Sept. 17, the Salmon Arm woman underwent a Deep Brain Stimulation procedure in Vancouver for Parkinson’s Disease.
Thirteen years ago, at age 49, Kennah-Hafstein was in her prime as a chemistry and math teacher at Eagle River Secondary in Sicamous. That changed when she was diagnosed with Parkinson’s. She began taking medication to manage the symptoms almost immediately, but did not respond well to them.
In 2011 her neurologist suggested she consider Deep Brain Stimulation surgery (DBS). Eager to find alternatives to brain surgery, she began researching. Kennah-Hafstein tried a natural substance as an alternative to the pharmaceuticals, but the successes didn’t last.
In 2017 she was officially put on the wait list for DBS. Her symptoms got more severe, adding to her stress. If a person with Parkinson’s has to wait too long for surgery, their condition can deteriorate to a point where the surgery is no longer effective. She lobbied, with the support of her neurosurgeon, for shorter wait times.
Now back home, Kennah-Hafstein says her neurosurgeon, Dr. Christopher Honey, was very pleased with his placement of the two electrodes needed.
“This is the most important part of the whole process because their placement will determine the type and quality of the symptoms relief I can expect,” she says.
Read more: In this corner, hope
Read more: Salmon Arm woman fights for a life-changing surgery
She and her husband Irwin were excited to learn that they could get a sneak preview of some of the expected improvements within hours of having the surgery, even though the neural stimulator would not be turned on for six to eight weeks. She says the improvements are from the stimulation that happens during the surgery as the surgeon locates the best possible position for the two electrodes.
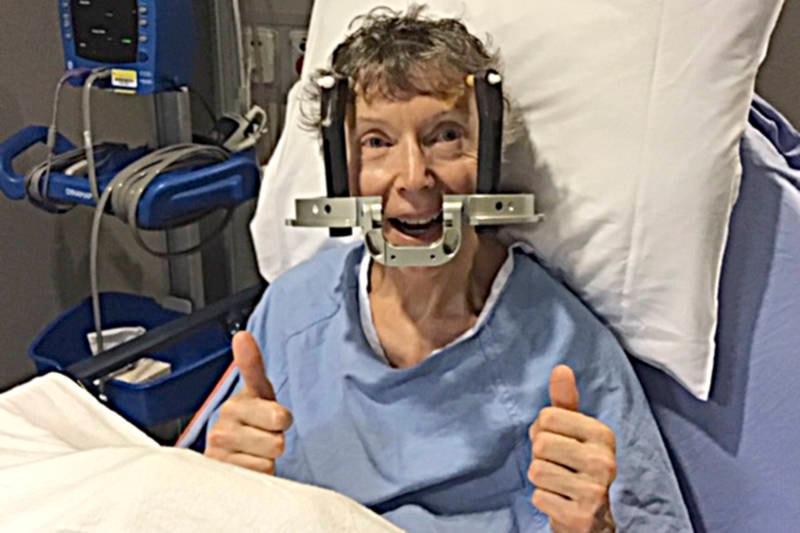
“Shortly after returning to my hospital room, my husband noticed that the excess body movements (dyskinesia) that caused me the most problems, were now completely gone. After years of watching me move, sometimes uncontrollably, sometimes all day long, he looked at me and said, ‘I’m liking this.’”
They knew it wouldn’t last but hoped it would stay for more than the couple of days predicted. It did.
“I was fortunate enough to experience the relief for a full two-and-a-half weeks after surgery,” she says, explaining she was also able to sleep in four-hour stretches rather than two.
Read more: Promised Parkinson’s surgery sparks hope for Salmon Arm woman
Read more: Shuswap woman with Parkinson’s receives long-awaited date for surgery
As for the surgery, she said it was more difficult to endure than she expected, and she greatly appreciated the support of the nurses who held her hands throughout.
“All I will say about the the actual reality of a surgery that involves drilling two holes in my head is that, they drilled two holes in my head.”
On Nov. 5, Kennah-Hafstein will return to Vancouver where the neural stimulator will be turned on for the first time.
“This marks another ‘beginning’ on my continuing journey with Parkinson’s Disease,” she says.
For the next six to eight weeks she will have weekly sessions at the DBS Clinic, where she will learn how to make adjustments to the stimulator to improve control of her symptoms, and her medication will be adjusted. She says it can take anywhere from a few weeks to six months until the adjustments are complete.
@SalmonArm
marthawickett@saobserver.net
Like us on Facebook and follow us on Twitter